Florida Perinatal Quality Collaborative
Past Projects

-
The PACC Initiative’s purpose was to work with providers, hospitals, and other stakeholders to improve maternal health through hospital facilitated continuum of postpartum care by arranging and providing respectful, timely, and risk-appropriate, coordinated care and services.
-
PAIRED was designed to help NICUs develop and implement unit-specific strategies that improve how a family engages with the NICU staff, to assist in the care of their infant in a way that provides value to the family and to the NICU team. As its centerpiece project, this initiative helped facilitate adoption or expansion of safe skin-to-skin care, which has a growing evidence base for achieving better infant and family outcomes.
-
The goal of the PROVIDE Initiative was to improve maternal and newborn outcomes by applying evidence-based interventions to promote primary vaginal deliveries at Florida delivery hospitals and ultimately reduce NTSV cesareans.
-
This project’s purpose was to work with providers, hospitals, and other stakeholders to improve identification, clinical care and coordinated treatment/support for pregnant women with opioid use disorder and their infants.
-
The purpose of this project was to work with Florida NICUs and stakeholders to standardize approaches to address variability in NAS management and decrease neonatal length of stay related to NAS.
-
The goal of this project was to work with Florida hospitals to improve hospital policies, procedures, and collaboration to increase access to immediate postpartum long-acting reversible contraception (LARC) usage, and to work with Medicaid, and other payers and state partners, to facilitate their use.
-
The Birth Certificate Improvement (BCI) Initiative's purpose was to improve the accuracy of birth certificate reporting for health care quality improvement and public health purposes. It ran from 2018 to 2019. As part of this work, FPQC has worked in conjunction with DOH to offer Birth Data Quality Training Workshops.
-
The aim of the Mother's Own Milk (MOM) project was to increase the number of very low birth weight (VLBW) infants in Florida who receive mothers' own milk at NICU discharge by focusing on intent to provide breast milk, establishing and maintaining mothers' supply, and transitioning to the breast.
-
The Hypertension in Pregnancy (HIP) Initiative launched in 2015, with participating of 32 Florida and 1 Colombia hospital. The project focused on reduction of short and long-term morbidity and mortality related to pregnancy hypertension; Proper screening, diagnosis and management of hypertensive disorders; Timely recognition and quick, organized response to preeclampsia; and Proper discharge screening and planning, including patient education. In 2017, this project entered a Sustainability Phase.
Sustaining HIP Standardization of Practice: Lessons and Success Stories
-
Since 2007, perinatal champions from five of the most populous states, CA, FL, IL, NY, and TX, which represent nearly 40% of the births in the U.S., have been working together to improve birth outcomes. Following the initial success of the Big 5 State early elective delivery pilot, (results published in Obstetrics and Gynecology Vol. 121, No. 5, May 2013) leaders launched the next Big 5 State initiative, improving the utilization of antenatal corticosteroids. Eleven Florida hospitals were involved in the March of Dimes ACT pilot.
- Proven reduction in neonatal morbidity and mortality
- Goal of 100% administration to at-risk mothers 23-34 weeks gestational age not being met
- Optimal timing of ACT 24 hours – 7 days prior to preterm delivery often not achieve
- Lack of standardized ACT protocols leads to inconsistent medical practice
- Poor documentation of ACT
- ACT is a PC-03 Joint Commission National Quality Measure
Materials
- March of Dimes ACT Passport
- March of Dimes Big 5 ACT Pilot Data Collection and Display Spreadsheet (Plan B)
- March of Dimes Big 5 ACT Hospital Transfer/Receiving Form
For ACT initiative resources, including the educational slide deck, algorithm, and key driver diagram, please visit PrematurityPrevention.org. You must create an account to download materials.
-
The successful transition from fetal to neonatal life involves many complex physiological changes. Interventions during this time period have been shown to have a great influence on a baby's future morbidities. Optimizing delivery room management of newborns provides many opportunities to impact outcomes positively with a lower occurrence of preventable illnesses.
The FPQC supported a "Golden Hour Part I: Delivery Room Management" quality improvement initiative for infants with a gestational age less than 30 6/7 weeks or birth weight less than 1500 grams. Through the guidance of the Lead Investigator - Maya Balakrishnan, MD, Assistant Professor, Department of Pediatrics, University of South Florida Morsani College of Medicine - and the active involvement of FPQC stakeholders, this Infant Health Advisory Subcommittee project team focused on teamwork, thermoregulation, oxygen saturation, and delayed cord clamping.
Evaluation Survey of Golden Hour Project Participants
TeamSTEPPS Training Video Clips
Read our publication on the Golden Hour Project in the Journal of Perinatology: Promoting teamwork may improve infant care processes during delivery room management: Florida perinatal quality collaborative’s approach (2017)
-
In order to address Florida's pregnancy-related mortality, the FPQC's maternal health advisors developed a Florida quality improvement Obstetric Hemorrhage Initiative (OHI) to address one of the largest and most preventable causes of maternal mortality in Florida.
-
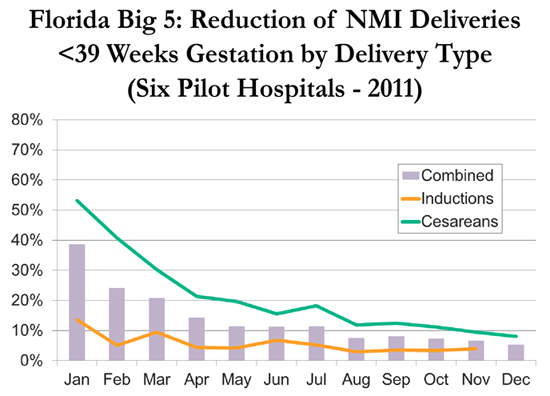
March of Dimes Big 5 Project: Reducing Non-Medically Indicated Deliveries (NMID) <39 Weeks
More than 30 years ago, the American Congress of Obstetricians and Gynecologists (ACOG) created guidelines advising obstetricians against elective deliveries without medical indications before 39 weeks gestation in order to improve the health outcomes of babies. According to ACOG, the last few weeks of a healthy pregnancy are necessary for the full development of some vital organs, such as the brain and lungs. Despite these guidelines, NMID <39 weeks gestational age steadily had been increasing in the United States by 2010 – with variability in the rates of such deliveries ranging from 5 - 40+%. At that time, the March of Dimes (MOD) decided to create a national collaborative comprised of the five most populous states – Florida, California, Texas, New York and Illinois – and to focus the Big 5 Collaborative’s first quality improvement (QI) initiative on eliminating NMID <39 weeks.
With a seed grant from the MOD to represent Florida, the FPQC focused its efforts on recruiting hospitals and educating practitioners. The FPQC and the MOD partnered to aid the efforts of six Florida hospitals in the Big 5 Hospital QI Project, a year-long pilot test of the “California Maternal Quality Care Collaborative Elimination of Non-Medically Indicated (Elective) Deliveries Before 39 Weeks Gestational Age” toolkit. The goal of the project was to change hospital policies and procedures to avoid scheduling these types of inductions or cesareans. To monitor project outcomes, data were collected on live births that were singleton, Florida residents and “term” pregnancies (370/7 – 386/7) with no medical conditions prior to or during pregnancies.
Each hospital was responsible for gathering together a QI team with a physician champion, nurse leader, scheduler and staff member. Without existing protocols in place, the hospitals’ QI teams were trained by the FPQC with the MOD on how to implement the California toolkit. Training included:
- Establishing consistent policies and procedures for scheduling guidelines
- Creating a uniform scheduling form
- Applying a “Hard Stop” policy process
- Collecting and inputting data accurately into the MOD national web data portal
The FPQC also coordinated Grand Rounds and other educational and promotional opportunities to help gain more staff buy-in.
Between January and December 2011: The hospitals input their de-identified data from the scheduling forms into the data portal. Improvement was monitored by each hospital through monthly and quarterly reports as well as monthly phone calls with the MOD and the FPQC to check individual progress, compare status against others, share new ideas for enhancements and discuss challenges and opportunities.
The project was extremely effective, and the results were published by the MOD at the national level. To access the abstract for "A Multistate Quality Improvement Program to Decrease Elective Deliveries Before 39 Weeks Gestation," please click here.
The success of the project attracted the interest of the Florida Hospital Association (FHA) and others. With continued funding from the MOD and new funding from the FHA, the FPQC has started a current project expanding the initiative on eliminating early elective deliveries (EED) through the Health Engagement Network (HEN) to more Florida hospitals.
-
Building on the success of the FPQC’s partnership in the March of Dimes (MOD) 2011 Big 5 Project to reduce non-medically indicated deliveries <39 weeks, the FPQC expanded this initiative to more Florida hospitals by continuing to partner with the MOD and the Florida Hospital Association (FHA). The three organizations, through the Health Research & Educational Trust (HRET) Hospital Engagement Network (HEN), continued working together to assist participating hospitals in moving towards the goal of reducing EED to 3% or less by the initiative’s conclusion in December 2013. Additionally, the FPQC worked with ACOG District XII to reach out to hospitals not yet identified as working with the MOD or the HEN to provide support and technical assistance in addressing EED. Substantial progress has been made in Florida and around the county at reducing these early deliveries. Efforts then focused on those few hospitals needing to further reduce these early births to acceptable levels.
Reducing EED before 39 weeks gestational age is a priority focus area for the Centers for Medicare and Medicaid Services (CMS) because research has shown that by doing so mothers and babies have better health outcomes – including a reduced length of stay, reduced transfer to an intensified level of care and decreased financial costs to the system. Elimination of EED requires the education, training and support of all perinatal health-related practitioners, advocates, policymakers and payers as well as patients and their families.
As part of Florida's Campaign to Reduce Early Elective Deliveries, the FPQC interviewed Florida ACOG District XII Chair Robert Yelverton, MD and Vice Chair Karen Harris, MD, who say that "We Just Haven't Gone Far Enough". View the video here.
-
The FPQC is one of the original 9 state Collaboratives in the NCABSI initiative which began in December 2011 with the goal of reducing central line associated infections through the application of defined insertion and maintenance toolkits. This project was the FPQC’s first newborn QI initiative.
Sixteen Florida Level III NICUs signed on to implement the existing protocol utilized across the nine-state project for Phase I, which was completed in December 2012. During Phase I, the Florida NICUs provided a quarter of the data and had a substantial impact on the national progress of the project – with Florida outperforming the national average in certain key measures.
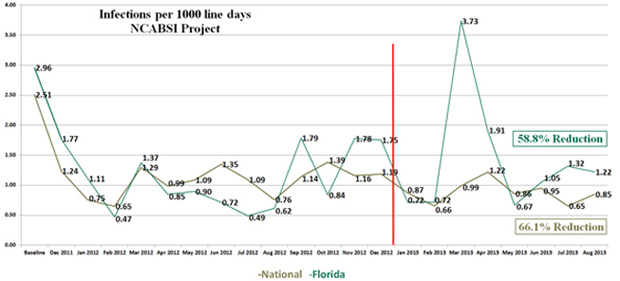
Phase II began in January 2013 (red line in figure) with the goal of maintaining the gains achieved in Phase I. The NCABSI project expanded nationally to include 13 states and over 150 NICUs. The 16 Florida NICUs involved have been the largest single data contributor, with over 7800 of the 40,000 lines and over 86,000 of the 376,000 line days.
Florida has reduced central line infection by over 58.8% by August 2013. Detailed results between December 2011 and August 2013 indicated that 150 infections were avoided in Florida - saving 18 lives, reducing length of stay by more than 1,199 days and saving over $7.9 million.
The effort included individual site visits by the state Lead Investigator, conference calls involving participating centers and a series of webinars on utilizing the American Hospital Association's Comprehensive Unit-Based Safety Program (CUSP) to achieve and sustain culture change. The spirit of cooperation and collaboration which grew out of this project will give Florida a strong foundation for future projects.
If you have any questions about this initiative, please contact Dr. Douglas E. Hardy at dehardy@icloud.com. For detailed information on the NCABSI initiative presented at the FPQC’s 2013 Annual Neonatal-Focused Meeting (September 2013), please click here. To view the NCABSI November 2013 update, please click here.